Measuring Quality in Healthcare is an activity that assesses a healthcare institution’s or providers’ performance in delivering highly effective, efficient and timely patient care and services.
Measuring quality will involve assessing and developing processes, outcomes, and organization. It usually involves specific characteristics such as:
- Data collection
- Evaluation
- Assessing Outcomes
- Assessing and developing efficiency
- Transparency
- Improvement
Measuring healthcare Quality can involve various methods, tools and metrics. Through assessing and improving quality, we can optimize performance against targeted outcomes, which helps ensure patients receive the best quality care.
In today’s article, we’ll be looking at how we measure Quality in healthcare and how we can use the results to help drive improvement activities. We’ll be covering
- What is Quality in Healthcare
- How do we measure Quality in healthcare
- Factors that contribute to Quality in healthcare:
- What are the challenges of measuring Quality in healthcare
- How do we measure improvement in the Quality of Healthcare
- Quality in healthcare vs Quality in Manufacturing
- Benefits of measuring Quality in healthcare
- Issues in measuring healthcare in Quality
What is Quality in Healthcare
Quality management is highly relevant in healthcare as it is in other industries.
As with manufacturing, where “quality” helps focus an organization on delivering high-quality products and services to its customers, the same is true within healthcare, where “quality” helps healthcare providers ensure patients receive consistently high levels of care.

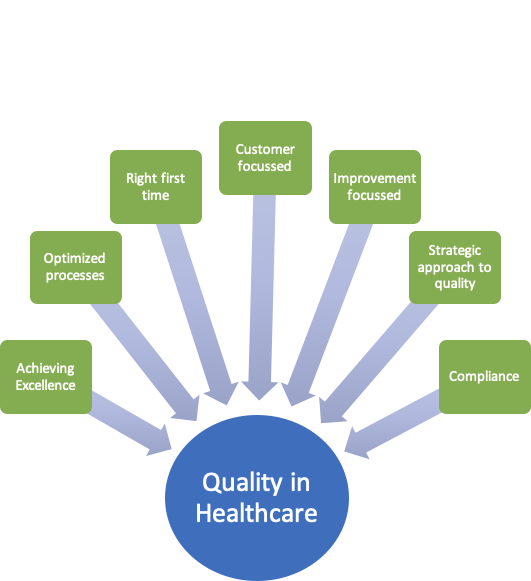
Healthcare institutions and providers utilize quality methodologies to achieve excellence, namely:
- Achieving excellence through high-quality outputs
- Optimizing processes
- Achieving right first time
- Developing an organization to be highly customer focussed
- Integrating continuous improvement into day-to-day operations
- Aligning Quality goals and objectives with the broader strategic approach
- Ensuring compliance with standards
In practice, that means benefits through:
- Focus on the patient (and patient satisfaction)
- Achieving desired clinical outcomes for patients
- Achieving high levels of safety
- Ensuring improvement focuses on levels of care
- Using data to measure and improve
- Maximizing Collaboration & Communication among providers
- Delivering high levels of process efficiency and effectiveness
- Timeliness of service delivery
How do we measure Quality in healthcare?
Healthcare can be an emotive concept, and it can be as much about perceived levels of quality as actual performance.
However, clinical metrics and indicators remain central to measuring the influence of quality and monitoring how processes and practices perform.
Like many industries, healthcare utilizes performance measures, in particular it uses them for three essential functions
- Driving improvement
- Ensuring accountability
- Providing a basis for research
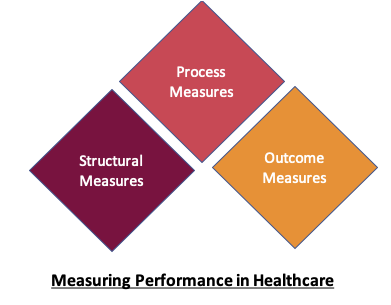
When it comes to Quality, the focus is principally on three key aspects
- Structural measures
- Process measures
- Outcome measures
Let’s take a deeper look at each:
Structural measures
Structural measures look to assess resources that help deliver healthcare services. This can include
- Capacity
- Systems
- Patient to provider ratio
- Organizational characteristics
- Resources that drive improvements
Process measures
Process measures, the most commonly used measures, focus on process effectiveness in lieu of the patient; examples include:
- Operational effectiveness
- Right first time (i.e. Medication errors)
- Diagnosis
- Compliance to policies
Outcome measures
Outcome measures analyze the results of healthcare services. This could include:
- Patient mortality
- Length of hospital stay
- Effect of healthcare on the population
- Patient Satisfaction
As we can see, many aspects of healthcare can be measured. As in other industries, some measurements are mandated by the applicable standards or regulations. Others are undertaken to ascertain performance levels.
As we stated at the beginning of this section, the perception of performance is key, primarily in order to develop patient trust but also in terms of capitalizing on funding lines. As a result, prioritization often features when undertaking assessments.
Performance, however, does not always equate to results, timelines can be met, and medication can be provided, but alas, patients don’t always recover.
As a result, measuring performance, particularly process performance and quality, can be complex.
Factors that contribute to Quality in healthcare
There are numerous factors that can contribute to the levels of healthcare quality.
It may come as no surprise that some are not particularly industry-specific and are common factors that influence quality in any sector.
However, healthcare does have some specific factors which are worthy of note.
Let’s take a look at some of the key influencing factors:
- Focus on the customer (in this instance, the patient)
- Appropriate and suitable education, qualification and training of healthcare staff at all levels
- Efficient, fact-based processes
- The adequate capacity of resources and equipment
- Collaboration between healthcare staff which focus’s on the optimization of patient care
- Continuous improvement embedded into working practices.
- Appropriate information strategy that plans and then uses data and information to maximize patient care (and does so whilst ensuring the privacy and confidentiality of patient records)
- Safe and clean environment for both patients and staff
- Timely provision of care to patients
- Healthcare is delivered right first time.
- Minimal errors in healthcare delivery
- Involving the patient in decision-making and method of healthcare delivery
As you can see, there are some common themes – customer-focused, effective processes, continuous improvement – these are universal when it comes to what drives quality.
What’s interesting is how these are applied – lead times are always important in discerning quality, but when it comes to health, timely access to care can have a significant impact on the patient – the same is true of reducing errors. When it comes to manufacturing, errors may result in a lot being scrapped; in healthcare, an error may lead to patient death.
When considering how we measure, healthcare professionals can employ a variety of methods. As ever, some are more applicable to certain circumstances than others; common methods include:
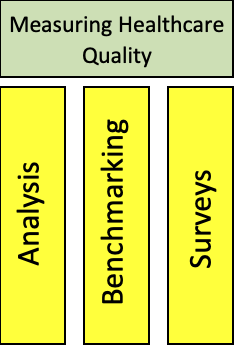
Data Analysis
There is a plethora of data available in healthcare, from patient records to computer systems and process records.
As with any industry, data analysis (in some cases statistical) form the basis for many assessments of performance.
Data needs to support three key measures (Structural, Process and Outcome and certain data may pertain to specific aspects (i.e. patient records are tied to process performance).
As ever, typical issues exist, including accuracy, availability, and complexity.
Benchmarking
Benchmarking helps healthcare providers compare themselves to others (either locally or beyond)
Healthcare providers can compare results against specific metrics, but this is reliant on having an appropriate set of peers against which results can be benchmarked.
As healthcare providers can vary in size and capability, it’s important to select an appropriate peer group when considering this method to ensure accurate (and actionable) results.
Surveys
Healthcare providers can utilize surveys in various circumstances, such as patient experience, in order to ascertain levels of performance. The results of surveys can ascertain performance and progress against improvement activities.
When utilizing surveys, there are a number of factors that should be considered, from the structure of questions being put forward to the sample size being surveyed.
What are the challenges of measuring quality in healthcare?
Perhaps the biggest challenge of healthcare quality is that, at its heart, it’s about human beings. As such, it’s unsurprising that it can be an emotive subject.
Whilst patient care and outcomes are a priority, there is a real danger that in describing typical quality methods (that, as quality professionals, we’re all familiar with), we imply that patients are the same as widgets on a shop floor.
As such, the approach is everything, and the patient/customer definitely comes first.
Another key issue is that healthcare provision is likely to involve a number of functions when looking at end-to-end patient care; as such, balancing differing perspectives and accountabilities is critical.
Other common challenges include:
- Selecting realistic goals and targets
- Balancing challenging cost and quality goals
- The need for transparency may impact behaviours, especially when faced with reporting poor performance (i.e. patient mortality levels)
- Clinical practice is complex, and finding appropriate methods of analyzing results may be challenging.
- Integrating data from multiple complex systems to adequately describe patient care may prove difficult.
How do we measure improvement in the Quality of Healthcare?
When assessing improvements, we can still apply our common PDCA process (Plan, Do, Check, Act) and our typical methodologies for driving change.
We can then measure improvement through three key steps.
- Have outcomes improved
- Impact on Metrics
- Impact of balancing measures (Have we implemented “improvements” that resulted in a detrimental impact in other parts of the system)
Delivering and measuring improvements is, of course, not without challenges, and we should still pay particular attention to
- Data issues which might impact our ability to measure change
- Our choice of metrics when trying to infer positive change.
- Transparency (or fear of personal or functional consequences)
- Access to tools that help us analyze situations to determine change
Quality in healthcare vs Quality in Manufacturing
As we can see, there are various similarities between Quality in healthcare and manufacturing – these include:
- Both focus on the customer.
- Compliance is central ((in manufacturing, this could mean adhering to specifications in healthcare clinical standards)
- Both integrate continuous improvement.
- Both involve analysis and metrics.
- Both involve balancing various aspects such as cost, efficiency and customer satisfaction.
Benefits of measuring Quality in healthcare
There are numerous benefits to having a quality-centred approach to healthcare; these include:
- Improved patient experience
- Optimized care that leads to improved recovery times
- Efficient use of resources (cost, people and equipment)
- Reputation of provider
- Optimized processes that can lead to both better patient outcomes and learning that can be shared with other providers
Issues in measuring healthcare in Quality
As a people-orientated service, delivering healthcare is fraught with challenges. There is a constant trade between the cost of care and the quality of care. As such, it’s unsurprising to find issues with how quality is both delivered and measured; these can include:
- Budget constraints may impact the effectiveness of delivery.
- Fragmented buy-in common
- Decision-making may be led by emotion, not fact
- Evolving Patient Needs may make measuring quality challenging
- Scarcity of certain resources
- Cultural variations
- Challenges of integrating multiple technologies that help deliver care
Summary
Measuring quality in any industry can be complex; there are additional aspects to healthcare that make it so, from the fact that outcomes can have a direct impact on people’s lives to the levels of expectation that the general public has around healthcare delivery.
There are tried and tested methods of providing, assessing and improving quality in healthcare, whether they’re focused on outcomes, regulatory compliance or cost-effectiveness.
Measuring quality requires a range of approaches and strategies, which may involve a range of data and information sources (some of which, such as patient clinical records, may bring their own challenges).
Whatever the approach, ensuring a focused approach to the delivery and measurement of quality can have significant benefits to the customer/patient and users of healthcare systems.
As ever, we’d love your feedback, particularly if you’re involved in delivering quality within a healthcare environment; you can reach us on Twitter or via the comments section below.
